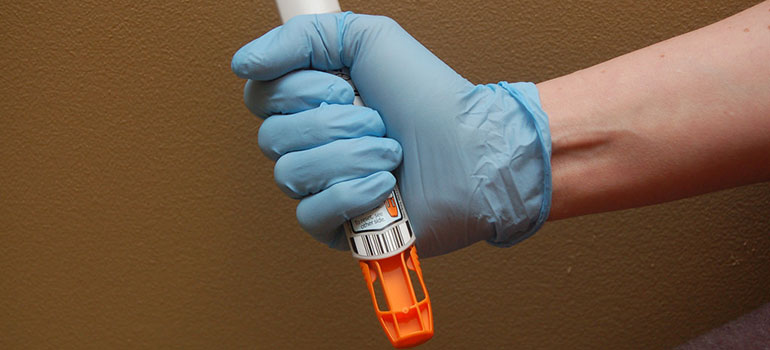
Autoinjectors like EpiPens—which contain the drug epinephrine—are crucial to treating anaphylaxis, a severe reaction usually due to an allergy that can cause a dramatic drop in blood pressure, narrowing of the airways or vomiting.
But Dr. Edmond Chan, head of the division of allergy and immunology in UBC’s department of pediatrics and director of the Allergy Clinic at BC Children’s Hospital, was troubled by the number of children brought to the emergency department with untreated anaphylaxis, even though the parents had an autoinjector handy.
This inspired Chan to design a first-of-its-kind experiment that put parents to the test at the moment of anaphylaxis for their child, described in this month’s issue of Annals of Allergy, Asthma and Immunology.
How did you measure parents’ knowledge of using autoinjectors?
Typically, when we think a child might have outgrown a food allergy, we schedule an “oral food challenge”— deliberately exposing them, under close supervision, to the food that they were allergic to. In general, there is a 30 per cent to 50 per cent chance they will still have a reaction, and about a 5 per cent to 10 per cent chance of anaphylaxis. So we decided to harness those sessions as a teaching moment. If the child went into anaphylaxis, we wanted to see whether the parents realized it, and how they handled it.
How did the parents perform?
Not as well as one would hope. We had 18 cases where epinephrine was needed, and many parents weren’t able to recognize the signs. When it came to actually using the autoinjector, they didn’t do much better. Some of them held it backwards, put their thumb over the needle, or didn’t inject the autoinjector long enough. These devices are deliberately made to be user-friendly, so we were surprised. The findings are concerning especially considering how dangerous anaphylaxis can be.
What do you make of those results?
The training that parents receive is not sufficient. Some physicians and pharmacists run through it very quickly, using a practice device that doesn’t have a needle. And even if the explanation is good, it’s probably difficult for stressed parents, in the throes of an anaphylactic crisis, to remember what they were told weeks, months or even years before. The parents themselves seemed to be aware of this – when we asked them before the food challenge about their confidence in administering the drug, the median score was three out of five. This is very troubling, because providing epinephrine early and properly could mean avoiding a reaction from becoming more severe, or even saving a child’s life.
Is there any good news from this study?
Certainly. The 18 parents or children who used the autoinjector for anaphylaxis during oral food challenges reported higher confidence after the challenge, with the median score rising from three to four. It was a clear demonstration that making someone perform a task in real-world conditions is more effective than telling them how to do it in a hypothetical scenario. Our study suggests we should routinely use food challenges, under controlled conditions, as teaching moments. And when children are brought to hospital in anaphylaxis, we should encourage nurses and physicians to hand an EpiPen to the parent and say, “On second thought, why don’t you do it?”
Note to reporters/editors/producers: Chan, along with a parent who used an autoinjector in the experiment, are available for interviews. Contact: Brian Kladko, Communications Manager, UBC Faculty of Medicine, at 778-838-4169 or 604-827-3301 or brian.kladko@ubc.ca